Delirium: Is Your Loved One at Risk?
Learn about the signs and symptoms of delirium, who is most at risk, and what you can do to help.
Start Lesson
Lesson Outline
Delirium is a condition that causes a person to become confused. It is not a specific disease itself; but is a change in a person's attention, awareness, and thinking. It develops over a short period of time and is caused by one or more other medical conditions or drugs. Delirium can be very frightening for the affected person and their family and friends. By reducing some of the risk factors that may cause delirium, it may be possible to prevent it.
By taking this interactive lesson, you’ll learn the answers to the following questions:
- What causes delirium?
- Who is at greatest risk of developing delirium?
- What are the signs and symptoms?
- How is it diagnosed and treated?
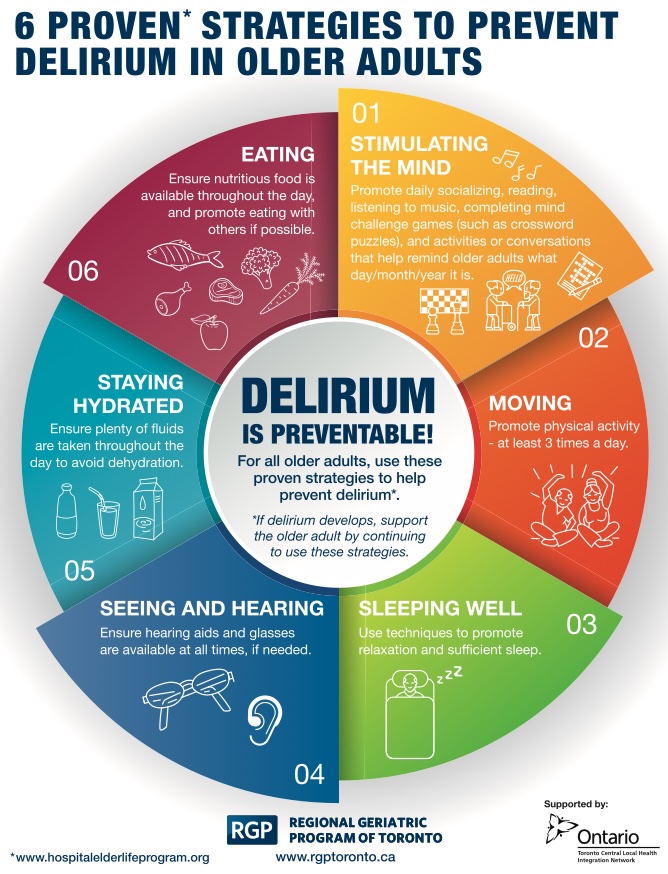
- What can be done to prevent it?
- How can family members help?
In this lesson, you'll meet Sebastian, who developed confusion while recovering from hip surgery. Find out what his family and healthcare team did to help him.
⏱ 15 minutes
Start LessonWhat is delirium?
Delirium is a sudden confused state of mind. It is not a specific disease itself; but a change in a person’s attention, awareness, and thinking. It develops over a short period of time and is caused by one or more other medical conditions or drugs. The signs and symptoms tend to fluctuate or vary throughout the day. Finding and trying to treat the underlying causes is key to trying to reverse the delirium. Delirium usually lasts about one week but can persist for longer. Most people with delirium have a full recovery. While delirium can happen to anyone, anywhere, it often occurs when someone is in the hospital.
People experiencing delirium may become more physically active or agitated (hyperactive), less active or sluggish (hypoactive), or have a mixed level of activity that changes throughout the day. They may not be able to understand when people are trying to help them. They may become angry with family or hospital or long-term care staff. They may start to think that everyone is against them or are trying to harm them. Some people with delirium may want to call the police to get help. Because of their confusion, they may also be at increased risk of falling and often experience emotional distress.
How is delirium treated?
Treatment depends on identifying and managing the cause or causes of the delirium. Whether at home, in the hospital or in another setting, it is important to keep the person safe and calm. Anyone with delirium should see a healthcare provider right away. The healthcare team will try to find the cause of the delirium and then address the factors or ease the symptoms. Depending on the cause, this could include:
- reviewing and changing medications
- providing fluids
- correcting chemical problems in the body
- treating infections, or
- treating low oxygen levels.
When the causes of delirium are managed, it often clears in a few days or weeks in many people; and most people will have a full recovery.

Related Resources
Authors
_jpg.jpg?sfvrsn=bcb0dd6_2)
Anthony J. Levinson, MD, MSc, FRCPC
Neuropsychiatrist; Professor; Director, Division of e-Learning Innovation, Faculty of Health Sciences, McMaster University
About this Project
This e-learning lesson was developed by the Division of e-Learning Innovation in the Faculty of Health Sciences. It was reviewed and assessed for accuracy by Dr. Anthony J. Levinson. There are no conflicts of interest.
The development process included a review of the Canadian Coalition for Seniors' Mental Health's 2014 Guideline Update on the assessment and treatment of delirium, Health Quality Ontario's conversation guide for family members of people with or at risk for delirium, and other relevant literature.
If you have questions or comments about this resource, please contact us at info@mcmasteroptimalaging.org.
References
- Burton JK, Craig L, Yong SQ, et al. Non-pharmacological interventions for preventing delirium in hospitalised non-ICU patients. Cochrane Database Syst Rev. 2021;2021(11). doi:10.1002/14651858.CD013307.pub3
- Francis J, Young GB. Patient Education: Delirium (Beyond the Basics). UpToDate. https://www.uptodate.com/contents/delirium-beyond-the-basics. Updated February 16, 2021. Accessed February 14. 2023.
- Gage L, Hogan DB. 2014 Canadian Coalition for Seniors’ Mental Health Guideline Update: The Assessment and Treatment of Delirium. https://ccsmh.ca/wp-content/uploads/2016/03/2014-ccsmh-Guideline-Update-Delirium.pdf. Published 2014. Accessed February 14, 2023.
- Hshieh TT, Inouye SK, Oh ES. Delirium in the Elderly. Clin Geriatr Med. 2020;36(2):183-199. doi:10.1016/j.cger.2019.11.001
- Inouye SK. Delirium-A Framework to Improve Acute Care for Older Persons. J Am Geriatr Soc. 2018;66(3):446-451. doi:10.1111/jgs.15296
- Ontario Health. Delirium Patient Guide. https://www.hqontario.ca/Portals/0/documents/evidence/quality-standards/qs-delirium-patient-guide-en.pdf. Published 2021. Accessed February 14, 2023.
- Ontario Health. Delirium Quality Standard. https://www.hqontario.ca/Portals/0/documents/evidence/quality-standards/qs-delirium-quality-standard-en.pdf. Published 2021. Accessed February 14, 2023.
- Patterson CJ. Recognize and prevent delirium (confusion and agitation) when in hospital. McMaster Optimal Aging Portal. https://www.mcmasteroptimalaging.org/blog/detail/blog/2014/03/14/delirium-what-is-it-and-can-we-prevent-it. Published March 14, 2014. Updated December 20, 2017. Accessed February 14, 2023.
Disclaimer